
♦ Antibiotics in the discs in the culture on the left prevent bacteria from proliferating.
♦ Bacteria in the culture on the right are resistant to most of the antibiotics.
Antibiotics kill certain types of bacteria. Over time, those bacteria change to develop resistance to the antibiotics. Called antibiotic resistance, this is one of the most serious problems facing modern surgery and medicine.[1][2][3] It is also one of the best examples of evolution in action. According to The Lancet, at least 1.2 million people died because of drug-resistant bacterial infections in 2019, more than from HIV or malaria.[4]
Antibiotic resistance spreads very quickly, far faster than microbiologists expected. "As long as new drugs keep coming, resistance is not a problem. But there has not been a new class of antibiotics discovered since the 1980s".[1] Some scientists have developed new antibiotics to combat resistant bacteria.[5][6] However, there is a lag-time of about eight years between discovery and possible availability for general use. The process is also extremely costly.[7]
The National Health Service is encouraging pharmaceutical companies to create new treatments by paying up to £20 million a year for new antibiotics no matter how many are prescribed, so they so they get paid even if the drugs are just kept in reserve for special cases or an emergency. [8]
Natural selection in action
[change | change source]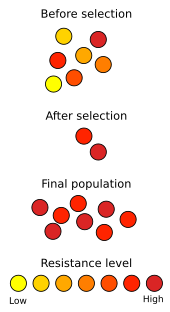
A well-known example of natural selection in action is the development of antibiotic resistance in microorganisms. Since the discovery of penicillin in 1928 by Alexander Fleming, antibiotics have been used to fight bacterial diseases. Natural populations of bacteria contain, among their vast numbers of individual members, considerable variation in their genetic material, as the result of mutations. When exposed to antibiotics, most bacteria die quickly, but some may have mutations that make them slightly less susceptible. If the exposure to antibiotics is short, these individuals will survive the treatment.
Prediction
[change | change source]In Fleming's 1945 Nobel Prize lecture he said:
- "It is not difficult to make microbes resistant to penicillin in the laboratory by exposing them to concentrations not sufficient to kill them, and the same thing has occasionally happened in the body... The time may come when penicillin can be bought by anyone in the shops. Then there is the danger that the ignorant man may easily underdose himself and by exposing his microbes to non-lethal quantities of the drug make them resistant".[9]
Mechanism
[change | change source]The mechanisms by which bacteria become antibiotic resistant are by genetic mutation and horizontal gene transfer. [10]
Effect on surgery and medicine
[change | change source]All surgery that involves cutting open the body poses massive risks of infection. Antibiotics given before and after surgery allow surgeons to do operations that would have been deadly before. Open-heart surgery is one obvious example.
Cancer treatments such as chemotherapy and radiotherapy damage the immune system. Antibiotics are prescribed to boost the body's natural defences. Patients with organ transplants always use drugs to suppress the immune system, otherwise it attacks the transplant. Therefore, antibiotics are used to protect the body. Without effective antibiotics, both sets of patients might die from infections which their immune systems could no longer control.
- "It's a pretty grim future, I think a lot of major surgery would be seriously threatened," said Professor Richard James of the University of Nottingham.[1]
Medical uses are also threatened. The number of tests coming back with resistance to carbapenems, one of the most powerful groups of antibiotics, has soared from a handful of cases in 2003 to more than 300 cases by 2010. "My lab is seeing an increasing number of resistant strains year on year," said Prof Neil Woodford, of the Health Protection Agency's antimicrobial resistance unit.[1] Most cases are resistant to some drugs. Even worse, there are a few cases of strains which no antibiotic can touch.
Many infections which were almost eliminated are coming back. The sexually transmitted disease gonorrhoea is becoming increasingly difficult to treat. Around the world, multi-drug resistant and extremely-drug resistant tuberculosis is a growing problem. Only a couple of drugs still work.
Infections that hit the elderly when they are in hospital are one of the main concerns. The greatest threat in the UK is opportunistic bugs which live in the gut such as E. coli and Klebsiella. They are now the most common form of infection which patients get in hospital. They show rising levels of resistance to antibiotics.
Official warnings
[change | change source]The UK Cabinet Office has issued a warning by the National Risk Register for Civil Emergencies. It says "the number of infections complicated by antimicrobial resistance could increase markedly over the next 20 years". "Without effective antibiotics, even minor surgery and routine operations could become high-risk procedures, leading to increased duration of illness and ultimately premature mortality".[11][12]
World Health Organization
[change | change source]The WHO has issued similar assessments:
- "The use and misuse of antimicrobials... over the past 70 years has led to a relentless rise in the number and types of microorganisms resistant to these medicines – leading to death, increased suffering and disability, and higher healthcare costs".[13]
- Deaths from acute respiratory infections, diarrhoeal diseases, measles, AIDS, malaria, and tuberculosis account for more than 85% of the mortality from infection worldwide. Resistance to first-line drugs in most of the pathogens causing these diseases ranges from zero to almost 100%. In some instances resistance to second- and thirdline agents is seriously compromising treatment outcome. The bacteria that cause tuberculosis (TB) can develop resistance to the antimicrobial drugs used to cure the disease. Multidrug-resistant TB (MDR-TB) is TB that does not respond to at least isoniazid and rifampicin, the 2 most powerful anti-TB drugs (WHO, 2018)
- "Added to this is the significant global burden of resistant, hospital-acquired infections, the emerging problems of antiviral resistance and the increasing problems of drug resistance in the neglected parasitic diseases of poor and marginalized populations".[14]
The WHO has now listed the world's most threatening superbugs.[15] Antibiotic resistant infections are being seen all over the world. In 2023 it said AMR has been associated with almost 5 million deaths a year and had cost the world $100 trillion in global economic losses.
Shareholders
[change | change source]About 70 per cent of antibiotics are given to farm animals to prevent disease. .Campaigners against misuse of antibiotics have raised the issue of antibiotics used in farming at company meetings, especially North American fast-food restaurant companies. [16]
Examples
[change | change source]Given enough time, and repeated exposure to the antibiotic, a population of antibiotic-resistant bacteria will emerge. This leads to what is known as an evolutionary arms race, or co-evolution, in which bacteria continue to develop strains that are less susceptible to antibiotics, while medical researchers continue to develop new antibiotics that can kill them.[17] A similar situation occurs with pesticide resistance in plants and insects, and with malarial resistance to quinine.
Gonorrhoea
[change | change source]A man in the UK has caught the "world's worst-ever case" of gonorrhoea, a sexually-transmitted disease. The main treatment by antibiotics azithromycin and ceftriaxone has failed to cure the disease.[18] An authority said "This is the first time a case has displayed such high-level resistance to both of these drugs and to most other commonly used antibiotics".
Methicillin-resistant Staphylococcus aureus
[change | change source]New strains of Methicillin-resistant Staphylococcus aureus (MRSA) have emerged that are resistant the next generation of drugs.[19]
Tuberculosis
[change | change source]Tuberculosis (TB) is an infectious disease caused by bacteria. It is caused by various types of mycobacteria, usually Mycobacterium tuberculosis. The disease usually attacks the lungs, but it can also affect other parts of the body. The pathogen can travel through the air, and spread from one person to the next. Experts believe that one third of the world population is infected with M. tuberculosis.[20] New infections occur at a rate of one per second.[20]
Drug-resistant TB is a serious public health issue in many developing countries, as its treatment is longer and requires more expensive drugs.[21] MDR-TB is defined as resistance to the two most effective first-line TB drugs: rifampicin and isoniazid. Extensively drug-resistant TB is also resistant to three or more of the six classes of second-line drugs.[22]
Totally drug-resistant TB was first observed in 2003 in Italy, but not widely reported until 2012. It is resistant to all currently used drugs.[23]
Malaria
[change | change source]Malaria infections are not caused by bacteria: they are caused by a protozoan parasite injected into the blood by a mosquito. They are normally treated by a combination of two drugs, artemether-lumefantrine. In 2017 four cases occurred in Britain where the drugs have failed. The patients got the disease in Africa. A doctor said "It is an early sign and we need to take it quite seriously as it may be snowballing into something with greater impact".[24]
Teixobactin
[change | change source]Teixobactin is an antibiotic discovered in 2015, the first new antibiotic discovered for forty years. It is not yet licensed for general use. It works against all gram-positive bacteria such as Staphylococcus aureus and against some other bacteria such as Mycobacterium tuberculosis.[25][26]
References
[change | change source]- ↑ 1.0 1.1 1.2 1.3 Gallagher, James 2015. Analysis: antibiotic apocalypse – is the end nigh? BBC News Health & Science. [1]
- ↑ Walsh, Fergus 2014. 'Golden age' of antibiotics 'set to end'. BBC News Science & Environment. [2]
- ↑ Roxby, Philippa. Millions are dying from drug-resistant infections, global report says. [3]
- ↑ "New bacterial 'dark matter' offers hope for a drug-resistant world | Financial Times". www.ft.com. Retrieved 2023-08-23.
- ↑ "New antibiotic effective against drug-resistant bacteria: First selective nucleoside-analog inhibitor of bacterial RNA polymerase". ScienceDaily. Retrieved 2017-10-09. According to Science Daily, "Scientists from Rutgers University-New Brunswick, the biotechnology company NAICONS Srl., and elsewhere have discovered a new antibiotic effective against drug-resistant bacteria: pseudouridimycin"
- ↑ Knapton, Sarah (2016-03-14). "First new antibiotic in 30 years discovered in major breakthrough". The Telegraph. ISSN 0307-1235. Retrieved 2017-10-09. A team from Northeastern University has "discovered a way of using an electronic chip to grow the microbes in the soil and then isolate their antibiotic chemical compounds. They discovered that one compound, Teixobactin, is highly effective against common bacterial infections Clostridium difficile, Mycobacterium tuberculous and Staphylococcus aureus".
- ↑ Paul, Steven M.; Mytelka, Daniel S.; Dunwiddie, Christopher T.; Persinger, Charles C.; Munos, Bernard H.; Lindborg, Stacy R.; Schacht, Aaron L. (2010). "How to improve R&D productivity: The pharmaceutical industry's grand challenge". Nature Reviews Drug Discovery. 9 (3): 203–14. doi:10.1038/nrd3078. PMID 20168317. S2CID 1299234.
- ↑ "NHS plans wider rollout of UK subscription model for antibiotics". Financial Times. 3 July 2023. Retrieved 10 July 2023.
- ↑ Fleming, Alexander 1945. Penicillin. Nobel lecture, p93
- ↑ Munita, J.M. (2016). "Mechanisms of antibiotic resistance". Microbiology Spectrum. 4 (2): 10.1128/microbiolspec.VMBF–0016–2015. doi:10.1128/microbiolspec.VMBF-0016-2015. PMC 4888801. PMID 27227291.
- ↑ National Risk Register for Civil Emergencies 2015 edition. HMSO. p15, 1.8 Antimicrobial resistance.
- ↑ Antibiotic resistance: 80,000 'might die' in future outbreak. BBC News 6.4.2015.
- ↑ World Health Organisation 2010
- ↑ WHO Global strategy for containment of antimicrobial resistance 2010
- ↑ Roberts, Michelle 2017. World's most threatening superbugs ranked in new list. BBC News [4]
- ↑ "Food companies face investor calls to curb antibiotic use on farms | Financial Times". www.ft.com. Retrieved 2023-08-22.
- ↑ "MRSA Superbug News". Archived from the original on 2006-04-26. Retrieved 2006-05-06.
- ↑ Gallagher, James 2018. Man has 'world's worst' super-gonorrhoea. BBC News Health. [5]
- ↑ Schito GC (2006). "The importance of the development of antibiotic resistance in Staphylococcus aureus". Clin Microbiol Infect. 12 (Suppl 1): 3–8. doi:10.1111/j.1469-0691.2006.01343.x. PMID 16445718. [6]
- ↑ 20.0 20.1 "Tuberculosis Fact sheet N°104". World Health Organization. November 2010. Retrieved 26 July 2011.
- ↑ O'Brien R (1994). "Drug-resistant tuberculosis: etiology, management and prevention". Semin Respir Infect. 9 (2): 104–12. PMID 7973169.
- ↑ Centers for Disease Control and Prevention (CDC) (2006). "Emergence of Mycobacterium tuberculosis with extensive resistance to second-line drugs—worldwide, 2000–2004". MMWR Morb Mortal Wkly Rep. 55 (11): 301–5. PMID 16557213.
- ↑ Maryn McKenna (2012). "Totally Resistant TB: earliest cases in Italy". Wired magazine. Retrieved 12 January 2012.
- ↑ Gallagher, James 2017. Malaria drugs fail for first time on patients in UK. BBC News [7]
- ↑ Gallagher, James 2015. Antibiotics: US discovery labelled 'game-changer' for medicine. BBC News Health. [8]
- ↑ Ling L.L. et al 2015. A new antibiotic kills pathogens without detectable resistance. Nature article preview. [9]