Structure
LRP5 is a transmembrane low-density lipoprotein receptor that shares a similar structure with LRP6. In each protein, about 85% of its 1600-amino-acid length is extracellular. Each has four β-propeller motifs at the amino terminal end that alternate with four epidermal growth factor (EGF)-like repeats. Most extracellular ligands bind to LRP5 and LRP6 at the β-propellers. Each protein has a single-pass, 22-amino-acid segment that crosses the cell membrane and a 207-amino-acid segment that is internal to the cell.[8]
Function
LRP5 acts as a co-receptor with LRP6 and the Frizzled protein family members for transducing signals by Wnt proteins through the canonical Wnt pathway.[8] This protein plays a key role in skeletal homeostasis.[7]
Transcription
The LRP5 promoter contains binding sites for KLF15 and SP1.[9] In addition, 5' region of the LRP5 gene contains four RUNX2 binding sites.[10] LRP5 has been shown in mice and humans to inhibit expression of TPH1, the rate-limiting biosynthetic enzyme for serotonin in enterochromaffin cells of the duodenum[11][12][13][14][15][16] and that excess plasma serotonin leads to inhibition in bone. On the other hand, one study in mouse has shown a direct effect of Lrp5 on bone.[17]
Interactions
LRP5 has been shown to interact with AXIN1.[18][19]
Canonical WNT signals are transduced through Frizzled receptor and LRP5/LRP6 coreceptor to downregulate GSK3beta (GSK3B) activity not depending on Ser-9 phosphorylation.[20] Reduction of canonical Wnt signals upon depletion of LRP5 and LRP6 results in p120-catenin degradation.[21]
Clinical significance
The Wnt signaling pathway was first linked to bone development when a loss-of-function mutation in LRP5 was found to cause osteoporosis-pseudoglioma syndrome.[22] Shortly thereafter, two studies reported that gain-of-function mutations in LRP5 caused high bone mass.[23][24] Many bone density related diseases are caused by mutations in the LRP5 gene. There is controversy whether bone grows through Lrp5 through bone or the intestine.[25] The majority of the current data supports the concept that bone mass is controlled by LRP5 through the osteocytes.[26] Mice with the same Lrp5 gain-of-function mutations as also have high bone mass.[27] The high bone mass is maintained when the mutation only occurs in limbs or in cells of the osteoblastic lineage.[17] Bone mechanotransduction occurs through Lrp5[28] and is suppressed if Lrp5 is removed in only osteocytes.[29] There are promising osteoporosis clinical trials targeting sclerostin, an osteocyte-specific protein which inhibits Wnt signaling by binding to Lrp5.[26][30] An alternative model that has been verified in mice and in humans is that Lrp5 controls bone formation by inhibiting expression of TPH1, the rate-limiting biosynthetic enzyme for serotonin, a molecule that regulates bone formation, in enterochromaffin cells of the duodenum[11][12][13][14][15][16] and that excess plasma serotonin leads to inhibition in bone. Another study found that a different Tph1-inhibitor decreased serotonin levels in the blood and intestine, but did not affect bone mass or markers of bone formation.[17]
LRP5 may be essential for the development of retinal vasculature, and may play a role in capillary maturation.[31] Mutations in this gene also cause familial exudative vitreoretinopathy.[7]
A glial-derived extracellular ligand, Norrin, acts on a transmembrane receptor, Frizzled4, a coreceptor, Lrp5, and an auxiliary membrane protein, TSPAN12, on the surface of developing endothelial cells to control a transcriptional program that regulates endothelial growth and maturation.[32]
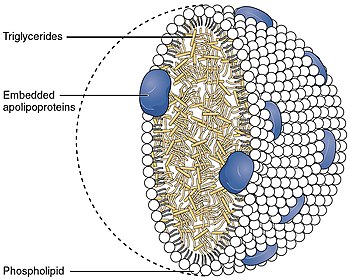
LRP5 knockout in mice led to increased plasma cholesterol levels on a high-fat diet because of the decreased hepatic clearance of chylomicron remnants. When fed a normal diet, LRP5-deficient mice showed a markedly impaired glucose tolerance with marked reduction in intracellular ATP and Ca2+ in response to glucose, and impairment in glucose-induced insulin secretion. IP3 production in response to glucose was also reduced in LRP5—islets possibly caused by a marked reduction of various transcripts for genes involved in glucose sensing in LRP5—islets. LRP5-deficient islets lacked the Wnt-3a-stimulated insulin secretion. These data suggest that WntLRP5 signaling contributes to the glucose-induced insulin secretion in the islets.[33]
In osteoarthritic chondrocytes the Wnt/beta-catenin pathway is activated with a significant up-regulation of beta-catenin mRNA expression. LRP5 mRNA and protein expression are also significantly up-regulated in osteoarthritic cartilage compared to normal cartilage, and LRP5 mRNA expression was further increased by vitamin D. Blocking LRP5 expression using siRNA against LRP5 resulted in a significant decrease in MMP13 mRNA and protein expressions. The catabolic role of LRP5 appears to be mediated by the Wnt/beta-catenin pathway in human osteoarthritis.[34]
The polyphenol curcumin increases the mRNA expression of LRP5.[35]
Mutations in LRP5 cause polycystic liver disease.[36]